What could ‘COVID season’ actually look like? | CBC News
This is an excerpt from Second Opinion, a weekly roundup of health and medical science news. If you haven’t subscribed yet, you can do that by clicking here.
As wave after wave of COVID-19 crashes over us, the hope is that we’ll eventually reach a point where seasonality of the virus will make the pandemic easier to predict and ride out.
But with highly contagious new variants emerging and driving surges around the world at different times — will we reach a regular “COVID season” anytime soon?
The pandemic hasn’t followed a clear-cut pattern in Canada, with waves hitting erratically in the spring, fall and winter over the past two and a half years, largely due to public health measures lifting and new variants threatening immunity from vaccines and prior infections.
- Do you have a coronavirus question or news tip for CBC News? Email us at ask@cbc.ca
Different variants have also caught countries off guard at unexpected times (and sometimes missed them altogether), making it increasingly challenging for us to predict when and where COVID waves would hit next.
“Let’s be honest, the virus is in control here, not us,” said Dr. Michael Gardam, an infectious diseases physician, medical director of infection prevention and control at Women’s College Hospital in Toronto and CEO of Health PEI.
“We’re entirely at the whim of whatever random evolutionary events occur and it’s really hard to predict.”
Different countries, different waves
Canada currently has a nasty mix of Omicron subvariants — including BA.1, BA.2, BA.2.12.1 and BA.2.3 — fuelling an ongoing sixth wave after public health measures were widely lifted, despite over 80 per cent of Canadians vaccinated and close to half the population infected.
The U.S. avoided a major BA.2 wave until late last month, but BA.2.12.1 is now quickly becoming the dominant strain at almost a third of new cases, while Europe is also contending with a surge in BA.2 subvariants and the emergence of BA.4 and BA.5.
That’s despite relatively high vaccination rates, with just over two-thirds double vaccinated in the U.S. and more than 70 per cent in Europe, and even higher levels of prior infection.
More than half of Americans had been infected with the virus as of February, according to new data from the U.S. Centers for Disease Control and Prevention, while EU officials reported between 60 and 80 per cent of the European population have had COVID-19.
“It is going to get increasingly difficult to compare countries … and honestly even before this it was kind of hard,” said University of Arizona immunologist Deepta Bhattacharya.
“The Alpha wave really nailed the U.K. and it didn’t really here and I don’t know why that is. It certainly got introduced here and it didn’t spread to the same extent and I have no idea why. So there’s all sorts of stuff that makes it very difficult to understand and predict.”

Population immunity could blunt future waves
Another factor that’s hard to predict is just how population immunity will change — and whether prior infections and high vaccination rates will protect, or wane over time.
Tulio de Oliveira, the director of South Africa’s Centre for Epidemic Response and Innovation, said South Africa has had a high level of population immunity with over 90 per cent estimated to have been previously infected, vaccinated or both.
“That’s one of the reasons why we believe that the big Omicron wave that we had didn’t translate to a very high number of hospitalizations and deaths,” he said.
“And BA.2, despite emerging and going on to dominate all the infections in South Africa, did not translate into an uptick of infection, which was very different in Europe, where they had a BA.1 wave followed by a BA.2 wave.”
That double whammy of Omicron’s BA.1 and BA.2 hit Canada hard as well, fuelling a devastating fifth wave late last year that subsided right as BA.2 sparked a smaller sixth wave in April — but it also drove up our levels of population immunity.
“It gives you a sense that the more people who are infected with this and are vaccinated, the better you are at weathering it,” said Gardam.
“The hope is it starts to become like the other coronaviruses that infect us every year that cause colds … and eventually it’s pretty hard for the virus to come up with something so novel that you haven’t seen part of it before.”
As a result, Omicron and its subvariants completely changed Canada’s immunity landscape over the past few months.
Previously, Canada was more in line with a country like South Korea given our high vaccination rates and previously low levels of prior infection, de Oliveira said, with much of the country seeing relatively low levels of COVID throughout the pandemic.
With Omicron, we were more similar to countries like South Africa and the U.S. with much higher levels of population immunity — but our high vaccination rate protected us.
“What that means is that potentially as new variants and subvariants of Omicron emerge … that may translate in a relatively high number of infections, but potentially not in a very high rate of hospitalization and death,” he said.
“Look at wave one, it was a very small wave but there were a lot of hospitalizations,” said Gardam. “Then finally Omicron hit and the spike in infections was insane, but the death rate never got as high as it did in earlier waves. So we are getting better at fighting this off.”
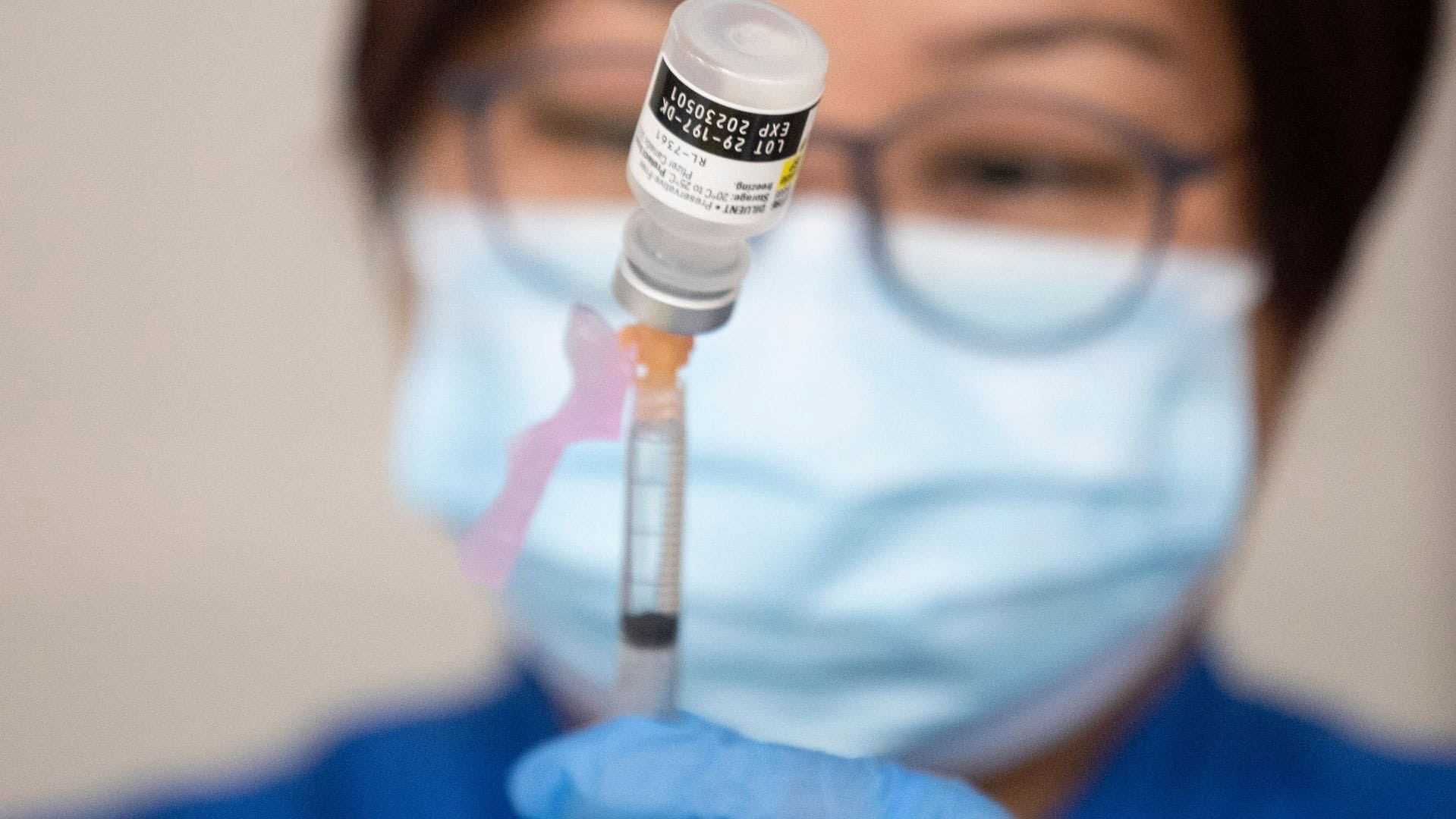
WATCH | Canadians urged to get COVID-19 booster shots to fight 6th wave:
All signs indicate Canada is going through a sixth pandemic wave, Dr. Theresa Tam confirms. Her message to Canadians: wear a mask and get boosted if eligible. 2:00
Gardam said the difference between provinces like Prince Edward Island and Ontario throughout the pandemic is that the Maritime provinces that took a COVID zero approach had little pre-existing immunity over the last two years.
But when Omicron hit in December, it exploited the province’s lack of population immunity.
“It was just like bang, here it is,” he said. “And it’s still going through the population and yet we had stricter measures than Ontario and other provinces did, but they had all these different waves going through that we didn’t have.”
How will we get to ‘COVID season’ with variants constantly emerging?
While it’s unclear if Canada’s newfound levels of population immunity and consistently high vaccination rates will fend off future waves of the virus and get us closer to seasonality, there are early hints from other countries that we may be able to better predict waves going forward.
Tom Wenseleers, an evolutionary biologist at Belgium’s KU Leuven University said on Twitter that South Africa is starting to show signs of seasonality with COVID, which could look like “a significant wave every six months with significant mortality and morbidity.”
The BA.4 & BA.5 Omicron subvariant-driven increase of new confirmed Covid cases in South Africa gives a good idea of what the endemic equilibrium will look like: a significant wave every 6 months with significant mortality & morbidity. 🧵 <a href=”https://t.co/I9jd5gMIPG”>pic.twitter.com/I9jd5gMIPG</a>
—@TWenseleers
“The impact on the healthcare system of both BA.2.12.1 and BA.4 and BA.5 is really not clear yet. They will cause waves of infections, for sure, but the impact on hospitalizations & expected mortality cannot yet be estimated at this time,” he told CBC News.
“The early data would seem to suggest similar severity as original Omicron in terms of case hospitalization ratio … but this is really early days to infer this.”
de Oliveira, who led the research team that identified subvariants BA.4 and BA.5 in South Africa, said waning immunity from infection and vaccination could factor into their spread.
“The only thing that may play a role in that is just the timing of the BA.1 wave, and that’s why we are looking very carefully at the data,” he said.
“We are talking about three or four months past the peak of BA.1 and we know around three or four months is when the population immunity starts decreasing.”
A new preprint study co-authored by de Oliveira, which has not yet been peer reviewed, suggested there could be “growth advantages” for BA.4 and BA.5 over BA.2 in South Africa that could potentially spark another wave, but whether that will happen there or in other countries remains to be seen.
And more variants are likely on the horizon.
“That just seems to be the behaviour of SARS-CoV-2 and I think that we shouldn’t be shocked when we see another variant,” said Alyson Kelvin, a virologist at the Canadian Center for Vaccinology and the Vaccine and Infectious Disease Organization in Saskatoon.
“But also keep planning for them, unfortunately, which I think, impacts our vaccination strategies … by the time you roll [an updated vaccine] out there’s a new variant.”

While Canada’s chaotic COVID wave pattern hasn’t shown major signs of seasonality yet, there are some indications we’re moving towards it.
“There still is seasonality associated with COVID. It doesn’t mean that it’s a perfect fit, but of course there are times during the colder months in Canada where we see more cases,” said Dr. Isaac Bogoch, an infectious diseases physician at Toronto General Hospital.
“Hopefully this wave will subside and we have a great summer ahead of us …. but can that be disrupted with a very transmissible variant? Maybe. It might.”
Gardam said if we look long-term at other viruses like H1N1, the flu strain that started the 1918 pandemic, we can expect COVID-19 to circulate for many years now that eliminating it altogether isn’t possible — but it likely won’t cause anywhere near the same level of illness.
“I have to assume that 20 years from now, there will be remnants of this coronavirus around that we get infected with regularly,” he said. “But it’s just not a big deal anymore.”
[ad_2]
Share this news on your Fb,Twitter and Whatsapp
NY Press News:Latest News Headlines
NY Press News||Health||New York||USA News||Technology||World News